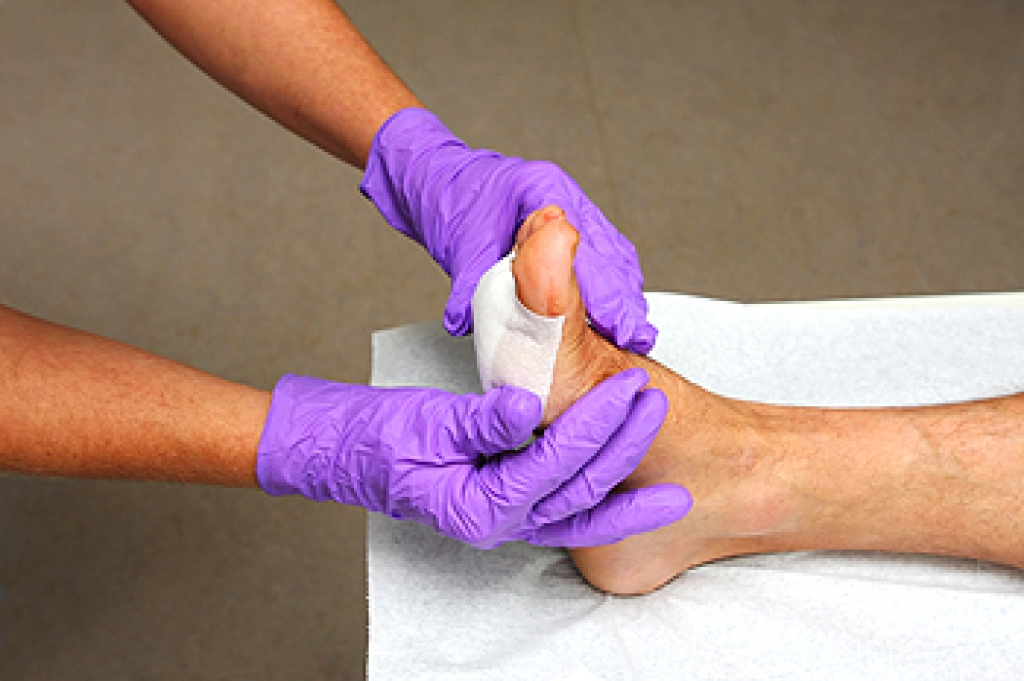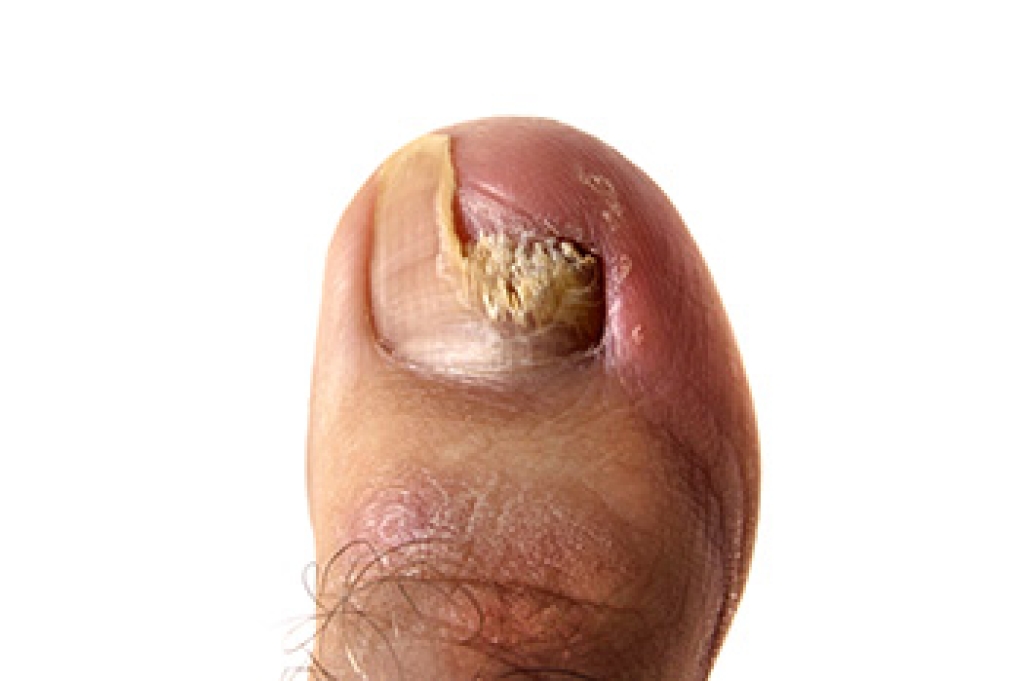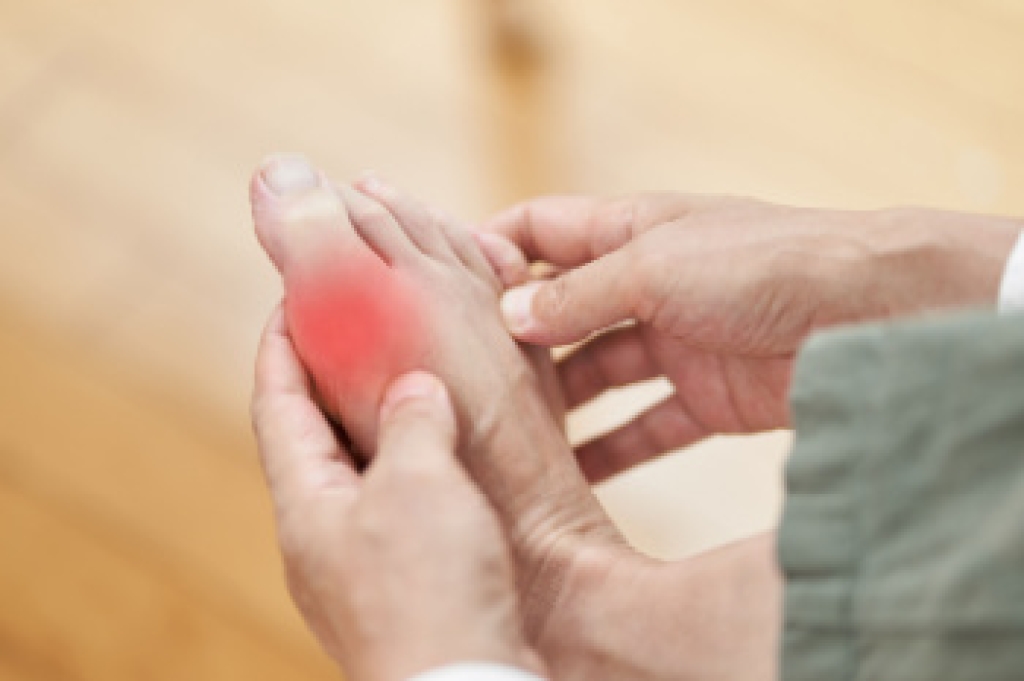
Gout is a form of arthritis that can cause sudden episodes of severe pain in the feet and ankles when uric acid crystals collect inside a joint. Gout frequently affects the big toe, but it may also involve the arch, heel, or ankle. During a flare-up, the joint may become swollen, stiff, and extremely sensitive. Skin often appears red or purple and feels warm to the touch. Some patients describe the pain as sharp, crushing, or pulsating, making it difficult to walk or wear shoes comfortably. Gout attacks may be the result of dehydration, alcohol use, certain medications, or diets high in purine-rich foods. Repeated inflammation can damage cartilage and surrounding tissue. A podiatrist can examine the painful area, evaluate joint changes, and help guide treatment to reduce inflammation and prevent future attacks. Care may include medication recommendations, footwear guidance, and strategies to reduce pressure on the affected joints. If you have symptoms of gout, it is suggested that you schedule an appointment with a podiatrist for relief and prevention tips from this painful condition.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Michael Schwartzman, DPM from Illinois and Indiana . Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions, please feel free to contact our offices located in West Chicago, IL and Whiting, IN . We offer the newest diagnostic and treatment technologies for all your foot care needs.